Are these stains decay?
Patients often come in to our office and ask if the stains in the grooves of their back teeth mean that they have decay and need to be filled. In fact, patients come in with a treatment plan from another dentist with numerous teeth that all of a sudden need fillings and the patient wants a second opinion. Although I wish I could say the decision to fill a tooth is a precise diagnosis that can be easily made and will be the same for all patients and dentists, I can not. Sometimes I agree with the treatment plan and sometimes I do not. The decision to drill and fill stains in the grooves of teeth has changed over time, varies with each patient, and is often a judgement call made by the dentist based on numerous factors including education, practice philosophy, and experience.
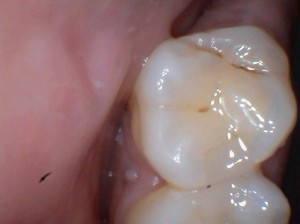 Why are the grooves stained?
Why are the grooves stained?
The grooves of the teeth are created during the formation of the tooth. These grooves can be so narrow that food/bacteria can stick in the teeth and cause a slight “melting”/demineralization into which color from food or bacterial products can become lodged. This early demineralization is the beginning of decay. If the process stops or remineralizes the groove is left with a “permanent” stain. If the groove continues to demineralize the bacteria invade the tooth and decay occurs. Sometimes superficial stains can just be polished away during a professional cleaning, while other times the decay may extend into the nerve. Monitoring stains to ensure decay does not progress is one of our most important duties as dentists and requires diligence and follow up.
Current treatment philosophies and research
Not long ago every groove with a stain was considered at risk and was drilled out and filled. Additionally, the treatment philosophy and materials required that any groove near the decay should be drilled out even if it was unaffected by decay. This was called “extension for prevention” and resulted in many of the large silver fillings that we see today. This was what I was taught in dental school in 1976 and I can remember even then my hesitation to remove those grooves; it seemed like such a waste of good tooth structure. Luckily, as many of you know, my nature is to question, and I began to study and change how I dealt with decay as soon as I left dental school.
This older treatment philosphy followed the medical surgical model that taught excison was the best treatment for disease. It did not take into account the bodies ability to heal or the fluid nature of the reparative process of teeth in the mouth. Decay or demineralizaton was considered a one way disease process that could only be dealt with by removal and replacement.
Fast forward to today where the focus has shifted from the drill, fill, and bill model to prevention and remineralization techniques. Now the question becomes: Do we have to fill or can we enable the tooth to remineralize? What are the risk factors causing the disease, and how can we control them? What preventive techniques can we use to stop the decay process? Simply put, a cavity doesn’t always have to get worse. Certainly, there is a point of no return, but dentistry has been adjusting this point as new research shows remineralization can and does reverse the decay process. Much depends on the patients’s ability to keep the area clean, to reduce the acidity in their mouth, and to reduce the amount of sugar available for the bacteria to produce acid. If the decay has not created an area that is impossible to clean, then remineralization has a chance.
How does a dentist find decay and determine its depth?
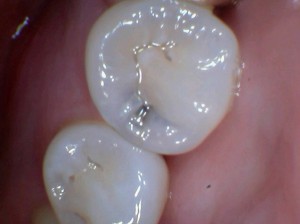 The most obvious way is simply looking at the teeth, the depth of the stain, the position of the stain, and the character of the stain. We use magnification, intense lights, and the explorer or probe. With bright illumination the depth and width of the stain can be seen through the enamel and can help us to determine if the decay has reached the softer portion of the tooth. The stains in some areas of the teeth are more likely to be decay, often in areas where cleaning is especially difficult because the groove is so deep or access is difficult. The dentist uses his experience to make a decision about the aggressiveness of the decay, which I describe as the character of the stain. It is not something easily described, it is almost a feeling based on color and texture. The thought process often goes: I’ve seen decay like this before and it wasn’t good, or I’ve seen stain similar to this and it did not change for years. Thirty two years of experience gives me a wealth of previous situations to draw from. Have I always been right? No, but I care about every tooth and each patient, always making sure they understand the risks, benefits and decision making process.
The most obvious way is simply looking at the teeth, the depth of the stain, the position of the stain, and the character of the stain. We use magnification, intense lights, and the explorer or probe. With bright illumination the depth and width of the stain can be seen through the enamel and can help us to determine if the decay has reached the softer portion of the tooth. The stains in some areas of the teeth are more likely to be decay, often in areas where cleaning is especially difficult because the groove is so deep or access is difficult. The dentist uses his experience to make a decision about the aggressiveness of the decay, which I describe as the character of the stain. It is not something easily described, it is almost a feeling based on color and texture. The thought process often goes: I’ve seen decay like this before and it wasn’t good, or I’ve seen stain similar to this and it did not change for years. Thirty two years of experience gives me a wealth of previous situations to draw from. Have I always been right? No, but I care about every tooth and each patient, always making sure they understand the risks, benefits and decision making process.
Tools to determine decay that needs to be filled vs stain that can be monitored.
The explorer is the most common tool and enables us to feel if the enamel has been softened to the point that it collapses and can be penetrated. Almost all of us have all been in the chair and know that sickening feeling when the explorer sticks in the tooth. Today, it doesn’t necessarily mean you have to have a filling, but it is still not a good sign.
Radiographs or xrays give us additional information about the depth of decay between the teeth, but they are not as useful for decay in the surface grooves. The new digital xrays do have enhancement tools and enable us to demonstrate to the patient with better visuals where the problems exist.
New tools using lazers and light reflection are being developed to detect decay. They claim to help the dentist by quantifying the decay, but can be affected by plaque, fillings and even moisture. Additionally, they have been shown to give false positives, unnecessarily indicating the need for a filling. With all of these tools, the manufaturers advise the dentist make the decision based on his experience not just the machine’s readings. The fact that you can find numerous listings for these expensive machines for sale used on ebay and other sites indicates that acceptance by dentists is not universal. We have not embraced this technology yet, but we are studying its efficacy.
Patient factors that determine the need for treatment.
Yes there is a person attached to the teeth and they have significant effect on the decision whether a tooth needs a filling or the if stain can be monitored. Ultimately, the decision is up to the patient. The question is: Can we expect the tooth to remineralize or at least not get worse before the next time we check it?
Habits and health
A patients habits can have a significant effect on the decay process. We have a list of questions regarding habits that factor into the decision monitor vs. filling. These factors include: sugar intake, soda consumption, smoking etc. The higher the sugar intake, the more likely the need for a filling. We also evaluate the patients desire to change and contribute to slowing the process. Often times simply stopping a cavity producing habit can stop the drill, fill, bill cycle. Of course, improving oral hygiene by increasing flossing, efficient brushing, or adding a remineralizing regimine can also reduce or reverse the decay process.
The patients health and medications can effect the decay process. As an example, acid reflux can add to the decay process, and many medications can reduce saliva which increases the speed of decay.
The age of the patient also effects our decision as dentists. A stain in a teenager’s tooth is much more of a concern than a stain in an eigthty year old person’s tooth. You have to figure, if the tooth has been in the mouth for seventy years without a filling, does it really need one now? A teenager’s softer teeth and poor diet make them much more suseptible to rapid decay…in addition to issues of compliance and rebellious tendencies.
Family history
I have the advantage of knowing families for years, some for over thiry years. We have grown up together, and I have treated grandparents, parents, grandchildren and great grandchildren. I have observed over time the family chemistry and the anatomy of their teeth, and, yes, some people just have better teeth. This information can be invaluable in determining whether we can monitor or have to fill a stain. I try not to give teeanagers another thing that they can blame on their parents, but I do let them know that they may get more cavities because this is their life and family trait.
Individual character
I know I can’t predict the future or whether a patient will change their habits. I know how difficult it is to change from my own experience as a dental patient. I was what I would call a “difficult” case. I am happy to say that we are able to communicate with our patients and often get them to understand the importance of their involvement in the process. We ask ourselves these questions:
- Does the patient care?
- Will the patient listen?
- Will the patient follow our reccommendation?
- Will the patient return for follow up monitoring?
The more “No’s” the more likely a filling would be the best reccommendation because it would better to fill before it gets any bigger. Some would say just drill a hole on all these areas before the decay gets bigger. I still marvel at the beauty of a virgin tooth without any fillings. I also know that once a filing has been placed, sooner or later it will need to be replaced, usually with a larger filling.
The Final Decision
So it is hard when a patient comes in one time and asks the question: “Should I have all these teeth filled?” I try to take into account all these factors explaining the risks and benefits of each course of action. I admit my faith in people makes me more conservative in my treatment recommendations.
